Read by 72 users
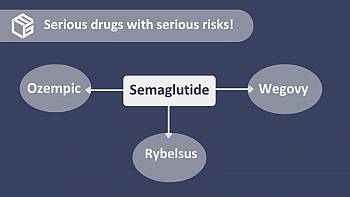
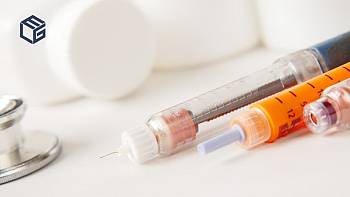
Ozempic use can result in concerning side effects – what you need to know about adverse reactions and stomach paralysisRead by 367 users
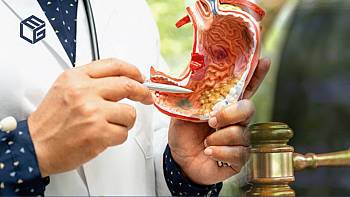
Ozempic manufacturer Novo Nordisk faces dozens of lawsuits filed by individuals affected by stomach paralysisRead by 1615 users
The reopening of the VCF allows 9/11 survivors and responders to obtain financial compensationRead by 1935 users
Individuals living near military bases contaminated with PFAS might also be eligible to file a claimRead by 1644 users
The importance of monitoring your health as a Camp Lejeune veteran or family memberRead by 1180 users
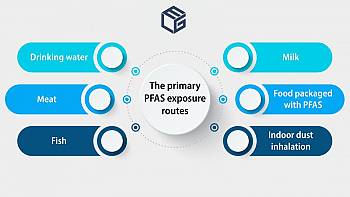
Black and Latino communities, disproportionately affected by drinking water with PFASRead by 825 users
Effectiveness of reverse osmosis filtration in removing PFAS: ensuring safe water reuseRead by 2128 users
Forever chemicals on trial: decoding a decade of contaminated waters and corporate accountability